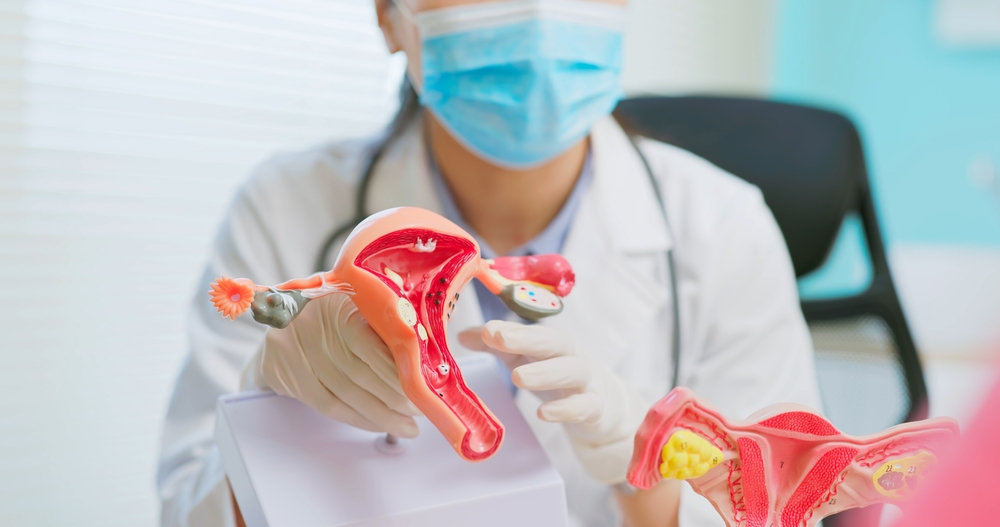
Many women living with polycystic ovary syndrome (PCOS) also struggle with persistent fatigue that interferes with daily life. While PCOS is widely known for symptoms such as irregular periods, acne, and weight changes, chronic fatigue is an often overlooked but very real concern for many patients.
When hormonal imbalances, metabolic changes, and inflammation associated with PCOS affect the body’s ability to regulate energy, chronic fatigue can develop. Understanding how these two conditions are connected is an important step toward finding effective treatment and improving overall health.
Through an integrative medicine approach, practitioners can evaluate the underlying drivers of both PCOS and chronic fatigue and develop personalized strategies to restore balance in the body.
What Is PCOS?
Polycystic ovary syndrome (PCOS) is one of the most common hormonal disorders affecting women of reproductive age. It occurs when the ovaries produce higher-than-normal levels of androgens, which are hormones typically associated with male physiology but also present in women.
These hormonal imbalances can disrupt the menstrual cycle and interfere with normal ovulation. PCOS is not, however, simply a reproductive condition. It is a complex metabolic and endocrine disorder that affects multiple systems throughout the body.
PCOS symptoms vary widely from person to person, but some of the most common include the following:
- Irregular or missed menstrual cycles
- Acne or oily skin
- Excess facial or body hair
- Weight gain or difficulty losing weight
- Insulin resistance
- Thinning hair on the scalp
- Fertility challenges
- Mood changes
- Persistent fatigue
Because PCOS affects hormone regulation, metabolism, and inflammation, it can have far-reaching effects on energy levels and overall well-being.
What Is Chronic Fatigue?
Chronic fatigue refers to persistent and overwhelming exhaustion that does not improve with rest. Unlike normal tiredness after a busy day, chronic fatigue can affect physical stamina, mental clarity, and emotional health.
People experiencing chronic fatigue often describe symptoms such as the following:
- Constant low energy
- Brain fog or difficulty concentrating
- Poor exercise tolerance
- Sleep disturbances
- Muscle weakness
- Increased sensitivity to stress
Fatigue can have many possible causes, including hormonal imbalances, nutrient deficiencies, immune dysfunction, and metabolic disturbances. In individuals with PCOS, several of these factors may occur simultaneously.
Why PCOS Often Causes Fatigue
Many people assume that chronic fatigue in PCOS is simply due to poor sleep or stress. However, the biological mechanisms behind PCOS can directly disrupt the body’s energy systems. Several physiological factors connect PCOS with chronic fatigue:
Insulin Resistance
One of the most common metabolic issues associated with PCOS is insulin resistance. Insulin is a hormone that helps regulate blood sugar by allowing cells to use glucose for energy. When the body becomes resistant to insulin, cells cannot efficiently absorb glucose. As a result, blood sugar levels rise while the cells themselves struggle to produce energy. This imbalance can cause…
- Energy crashes after meals
- Brain fog
- Increased hunger
- Weight gain
- Persistent fatigue
Insulin resistance is one of the primary reasons many individuals with PCOS feel constantly drained.
Hormonal Imbalances
Hormone fluctuations can significantly affect energy regulation. In PCOS, elevated androgen levels and disrupted reproductive hormones may interfere with normal metabolic processes. Hormones that may influence chronic fatigue in PCOS include the following:
- Estrogen
- Progesterone
- Testosterone
- Cortisol
- Thyroid hormones
For example, low progesterone levels associated with irregular ovulation may affect sleep quality. Meanwhile, stress-related cortisol imbalances can disrupt the body’s natural energy rhythms. When multiple hormone systems become dysregulated, fatigue often follows.
Chronic Inflammation
Research increasingly shows that PCOS is associated with low-grade chronic inflammation. Inflammation occurs when the immune system becomes activated in response to stressors in the body. While short-term inflammation is part of the healing process, long-term inflammation can interfere with normal cellular function. Inflammation may contribute to…
- Poor mitochondrial energy production
- Hormonal disruption
- Increased insulin resistance
- Fatigue and brain fog
This inflammatory environment makes it harder for the body to generate and sustain energy.
Nutrient Deficiencies
Individuals with PCOS may also experience nutrient deficiencies that impact energy production. Certain nutrients are essential for metabolism and mitochondrial function, including the following:
- Vitamin B12
- Vitamin D
- Magnesium
- Iron
- Omega-3 fatty acids
Low levels of these nutrients can worsen fatigue, impair cognitive function, and make it more difficult for the body to regulate hormones.
Sleep Disruptions
Sleep problems are surprisingly common in people with PCOS. Hormonal imbalances and metabolic disturbances can affect sleep quality in several ways. Some individuals with PCOS experience…
- Insomnia
- Restless sleep
- Sleep apnea
- Nighttime blood sugar fluctuations
When sleep becomes disrupted, the body has less opportunity to repair tissues, regulate hormones, and restore energy.
How Integrative Medicine Can Help PCOS and Fatigue
When addressing PCOS and chronic fatigue together, integrative care focuses on correcting the underlying imbalances driving both conditions through the following methods:
Comprehensive Lab Testing
Advanced laboratory testing can identify issues that contribute to fatigue in PCOS, including the following:
- Insulin resistance markers
- Hormone levels
- Thyroid function
- Nutrient deficiencies
- Inflammatory markers
These tests help guide targeted treatment plans rather than relying on generalized recommendations.
Metabolic and Blood Sugar Support
Improving insulin sensitivity is often a cornerstone of PCOS management. Strategies that support stable blood sugar may include the following:
- Nutrition plans focused on balanced macronutrients
- Targeted supplements that support insulin regulation
- Physical activity tailored to energy levels
When blood sugar becomes more stable, many individuals notice improvements in both energy and hormonal balance.
Hormone Optimization
Balancing hormones can also improve fatigue symptoms in PCOS. Depending on individual needs, treatment may focus on restoring healthy estrogen, progesterone, and androgen levels.
Improving hormone balance can support…
- Regular menstrual cycles
- Improved sleep quality
- Better mood and mental clarity
- Increased energy
Nutrient Repletion
Correcting nutrient deficiencies is another important step in restoring energy.
Integrative medicine practitioners often evaluate and support levels of nutrients such as the following:
- B vitamins for energy metabolism
- Vitamin D for immune and hormone support
- Magnesium for stress and sleep regulation
- Iron for oxygen transport
When the body has the nutrients it needs for cellular energy production, fatigue may gradually improve.
Stress and Lifestyle Support
Stress plays a significant role in both PCOS and fatigue. Chronic stress can disrupt cortisol rhythms, worsen insulin resistance, and impair sleep. Integrative treatment often includes strategies that help regulate the body’s stress response, including the following:
- Sleep optimization
- Stress-management techniques
- Gentle movement and exercise
- Mind-body therapies
Supporting these lifestyle factors helps restore the body’s natural balance and resilience.
A Root-Cause Approach to Energy and Hormonal Health
For many individuals, PCOS and chronic fatigue are deeply interconnected. Hormonal imbalances, metabolic dysfunction, inflammation, and nutrient deficiencies can create a cycle that leaves the body struggling to maintain energy.
By taking a root-cause approach, Hope for Healing aims to break this cycle. Rather than focusing solely on symptom management, this approach seeks to identify and correct the underlying factors driving both conditions. With the right evaluation and personalized care, many individuals can experience improvements in energy, hormonal balance, and overall well-being.If you are experiencing PCOS along with persistent fatigue, specialized care may help uncover the underlying causes and guide effective treatment. Learn more about care for PCOS and chronic fatigue here: https://get2theroot.com/chronic-fatigue